Spondylolisthesis and spondylolysis affect approximately 10% of the athletic population and 5 percent of the population in general. These conditions can cause back, buttock, and thigh pain, and even pain that radiates into the leg (below the knee) from compression of the spinal nerves. Most of the time, these conditions are asymptomatic and are an incidental finding on X-rays.
What is spondylolysis and spondylolisthesis?
There are two different types of spondylolysis and spondylolisthesis: isthmic and degenerative.
Isthmic spondylolysis & spondylolisthesis
Isthmic spondylolysis occurs when there is a stress fracture of the pars interarticularis, the bone that connects the facet joints in the spine (called “pars” for short). It may progress to the vertebrae slipping out of place if the fracture widens, leading to isthmic spondylolisthesis. The most common vertebral level for this condition is L5–S1 (in the lower back), but it can occur at any level.
Spondylolisthesis occurs when one vertebra (one of the bones in the spine) slips out of place onto the vertebra below it. Rarely appearing before age 8, isthmic spondylolisthesis can progress and in rare cases completely dislocate (this is known as spondyloptosis).
There may be a genetic predisposition to the pars fracture, as it is seen in up to 40% of Alaskan Indians. It is also commonly associated with a steep slope of the sacrum or a high pelvis. If the top of the sacrum is steeply sloped, there is much more shear stress on the pars interarticularis at L5. The sacral slope or pelvic incidence is determined by genetics and doesn't change with growth. The amount of slippage rarely progresses significantly in adulthood.
Degenerative spondylolisthesis
Degenerative spondylolisthesis typically becomes symptomatic in the middle-age and older populations. It most commonly occurs at the L4 - L5 vertebral level (the two lowest vertebrae in the lower back), but can occur at any level. With degenerative spondylolisthesis, there is no pars fracture. The facet joints in the back of the spine begin to wear over time, creating abnormal slippage onto the vertebra below. Because the posterior elements in the spine remain connected, small amounts of slippage can cause significant nerve compression.
Typical symptoms of degenerative spondylolisthesis include a decrease in standing and walking endurance. The body's response to the facet joint degeneration causes the ligaments to thicken, and large bone spurs may form in an attempt to prevent further slippage of the vertebrae. This response makes the nerve compression worse.
What are the treatment options for spondylolysis & spondylolisthesis?
Treatment options for spondylolysis and spondylolisthesis can vary based on the nature of the condition, the age of the patient, and the patient’s needs. Our specialists evaluate each patient individually to recommend the best course of action.
Treatments for degenerative spondylolisthesis
Non-operative treatment for degenerative spondylolisthesis includes anti-inflammatory medications, physical therapy, and sometimes epidural steroid injections.
When surgery is necessary, it almost always includes spinal fusion in addition to nerve decompression. The ligaments and facet spurs typically need to be removed to free the nerves, which further destabilizes an already unstable spinal motion segment. Fortunately, the outcome for this treatment is highly successful. Patients often notice an almost immediate Improvement in standing and walking endurance.
Treatments for isthmic spondylolysis & spondylolisthesis
Discovered in a growing child, we watch this condition carefully for progression and consider surgical treatment at a 50% slip. Typically, the condition is much more benign and rarely needs surgical treatment.
In adults, treatment is totally dependent on symptoms. Activity modification, bracing, anti-inflammatory medications, physical therapy, and sometimes epidural steroid injections are usually all that is needed. Physical therapy that avoids hyper-extension and centers on core strengthening tends to work best.
The type and extent of surgical treatment depends on the clinical symptoms and the patient's unique anatomy. Most commonly, it involves decompression of the nerves and surgical fusion of the unstable segment and possibly the segment above if it is involved. In young patients (usually under 30), if the disc is still normal and slippage hasn't occurred, we can directly repair and fix the pars defect to maintain motion in that segment of the spine.
Unfortunately, patients often do not have symptoms until the disc and motion segments wear out. Because of this, fusion is often the best choice. The good news is, as a group, these patients do well and are often able to return to full activity.
Patient examples: spondylolysis & spondylolisthesis
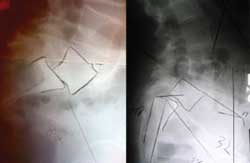
These two images are of different patients, both of whom have 50% slippage of the L5 vertebrae on the sacrum. They are very different cases and require different corrections to solve the patient’s problem. It is very important to differentiate these two when you are anticipating surgical correction. The first radiograph is of a typical isthmic spondylolisthesis. The second is one with lumbosacral kyphosis and is much more unstable. The second case will require sacropelvic realignment and pelvis fixation to maintain reduction.
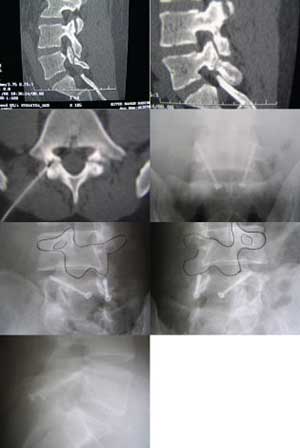
The next set of photos is from a teenage patient with a pars interarticularis fracture that didn't heal. In these rare cases where the L5-S1 disc is still normal, we elected to perform a direct screw repair of the pars defect and bone grafting. The pars defect healed, allowing for essentially normal motion in that segment of the spine.
The first two images show the fracture defect. The third image shows the defect being injected with local anesthetic. We did this as a diagnostic test. For several hours after the injection, the patient had complete relief of her pain.
Subsequent images show post-operative images with the screws bridging the defect. She is now back playing volleyball at a high level.
Spondylolysis & spondylolisthesis treatment in Austin, TX
Austin Spine offers a full range of treatment options for conditions like spondylolysis and spondylolisthesis in both adolescents and adults. If you would like to learn more about our treatment options, or would like to schedule an appointment with one of our specialists, please contact our office at (512) 347-7463.